|
1/14/2024 0 Comments Cyanokit hydroxocobalamin 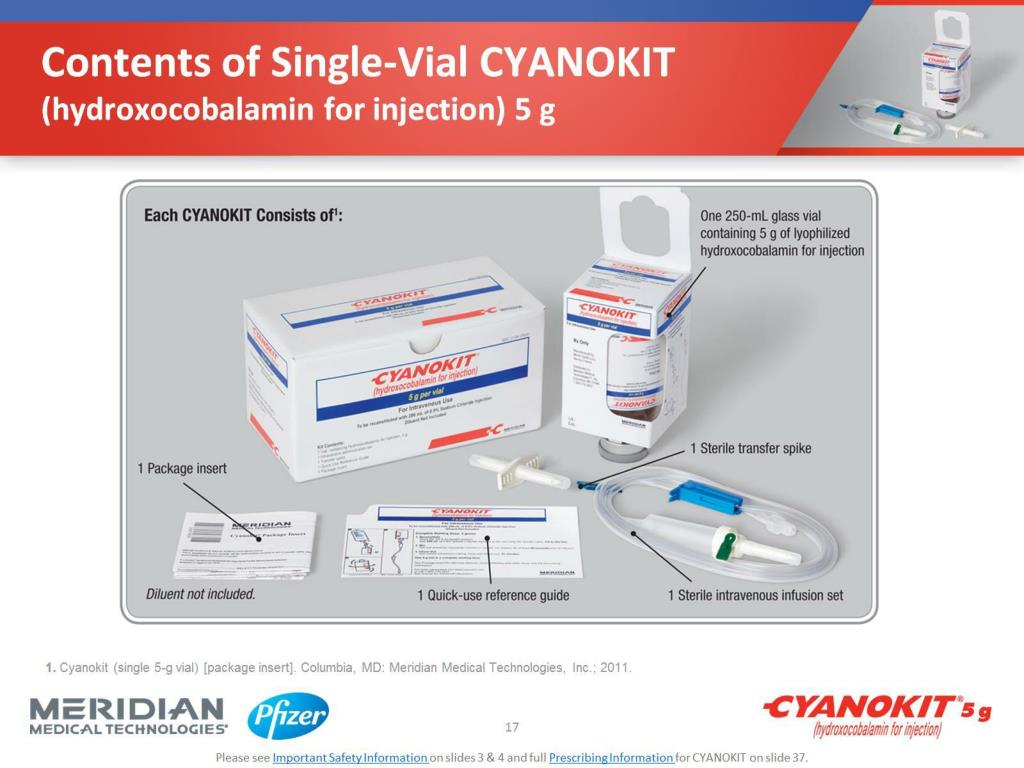
Fire victims: Hydroxocobalamin can discolor the skin and exudates, complicating the assessment of burn severity.Polycythemia vera: Vitamin B 12 deficiency masks signs of polycythemia vera vitamin B 12 administration may unmask this condition.Megaloblastic anemia: May mask previously unrecognized folate deficiency vitamin B 12 is not a substitute for folic acid.Thrombocytosis: Treatment of severe vitamin B 12 megaloblastic anemia may result in thrombocytosis.Renal injury: Renal injury, requiring hemodialysis for recovery in some cases, has been reported and may include acute renal failure with acute tubular necrosis, renal impairment, and urine calcium oxalate crystals monitor renal function for ≥7 days following therapy.Photosensitivity: May cause photosensitivity avoid direct sunlight while skin remains discolored.May offset hypotension induced by nitrite administration or cyanide monitor BP during treatment. Hypertension: Cyanide poisoning: Increased BP (≥180 mm Hg systolic or ≥110 mm Hg diastolic) may occur with infusion elevations usually noted at the beginning of the infusion, peak toward the end of the infusion, and return to baseline within 4 hours following the end of the infusion.Hypokalemia: According to the manufacturer, treatment of severe vitamin B 12 megaloblastic anemia may result in severe hypokalemia, sometimes fatal, due to intracellular potassium shift upon anemia resolution however, in more recent experience, while some patients may experience hypokalemia with initial treatment, it is transient and unlikely to be clinically significant (Carmel 2008).<1%, postmarketing, and/or case reports: Acute renal failure, acute tubular necrosis, angioedema, calcium oxalate nephrolithiasis (Legrand 2016), methemoglobinemia (Jiwani 2017), renal insufficiency Respiratory: Dry throat, dyspnea, pharyngeal edema Ophthalmic: Eye irritation, eye redness, swelling of eye Hypersensitivity: Hypersensitivity reaction Gastrointestinal: Abdominal distress, diarrhea, dyspepsia, dysphagia, hematochezia, vomiting Local: Infusion site reaction (6% to 39%)Ĭardiovascular: Chest discomfort, peripheral edemaĬentral nervous system: Dizziness, memory impairment, restlessness Hematologic & oncologic: Lymphocytopenia (8% to 17%) Genitourinary: Urine discoloration (100% may last up to 5 weeks after administration), calcium oxalate nephrolithiasis (56% to 61%) Miscellaneous: Swelling (feeling of swelling of the entire body)Ĭardiovascular: Increased blood pressure (18% to 28%)Ĭentral nervous system: Headache (6% to 33%)ĭermatologic: Erythema (94% to 100% may last up to 2 weeks), skin rash (20% to 44% predominantly acneiform eruption can appear 7 to 28 days after administration and usually resolves within a few weeks) Gastrointestinal: Diarrhea (mild, transient) The following adverse drug reactions and incidences are derived from product labeling unless otherwise specified.ĭermatologic: Pruritus, skin rash (transient) Mild symptoms or asymptomatic: IM: 1,000 mcg once weekly for 4 weeks maintenance dose: 1,000 mcg once every 2 to 3 months ( Ref).ĭuration of therapy: Continue indefinitely in patients with pernicious anemia or other irreversible cause of deficiency (eg, bariatric surgery) may discontinue therapy if a reversible cause of deficiency (eg, reduced dietary intake) has been addressed ( Ref). IM: 1,000 mcg every 3 months in patients with neurologic or neuropsychiatric symptoms, administer 1,000 mcg every 2 months ( Ref). Note: Continue parenteral therapy until the deficiency has been corrected and signs and symptoms have resolved before switching to oral therapy ( Ref). Alternatively, if neurologic symptoms are present, may initiate 1,000 mcg every other day for up to 3 weeks or until no further improvement in signs or symptoms, then switch to 1,000 mcg once weekly for up to 12 weeks ( Ref). Initial therapy: IM: 1,000 mcg every other day or once daily for 1 to 2 weeks, then 1,000 mcg once weekly for 4 to 8 weeks ( Ref). Severe/symptomatic anemia or neurologic/neuropsychiatric findings: Oral vitamin B 12 (eg, cyanocobalamin) may be used for less severe deficiency and/or maintenance therapy ( Ref). Note: Folic acid supplementation may also be required.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
